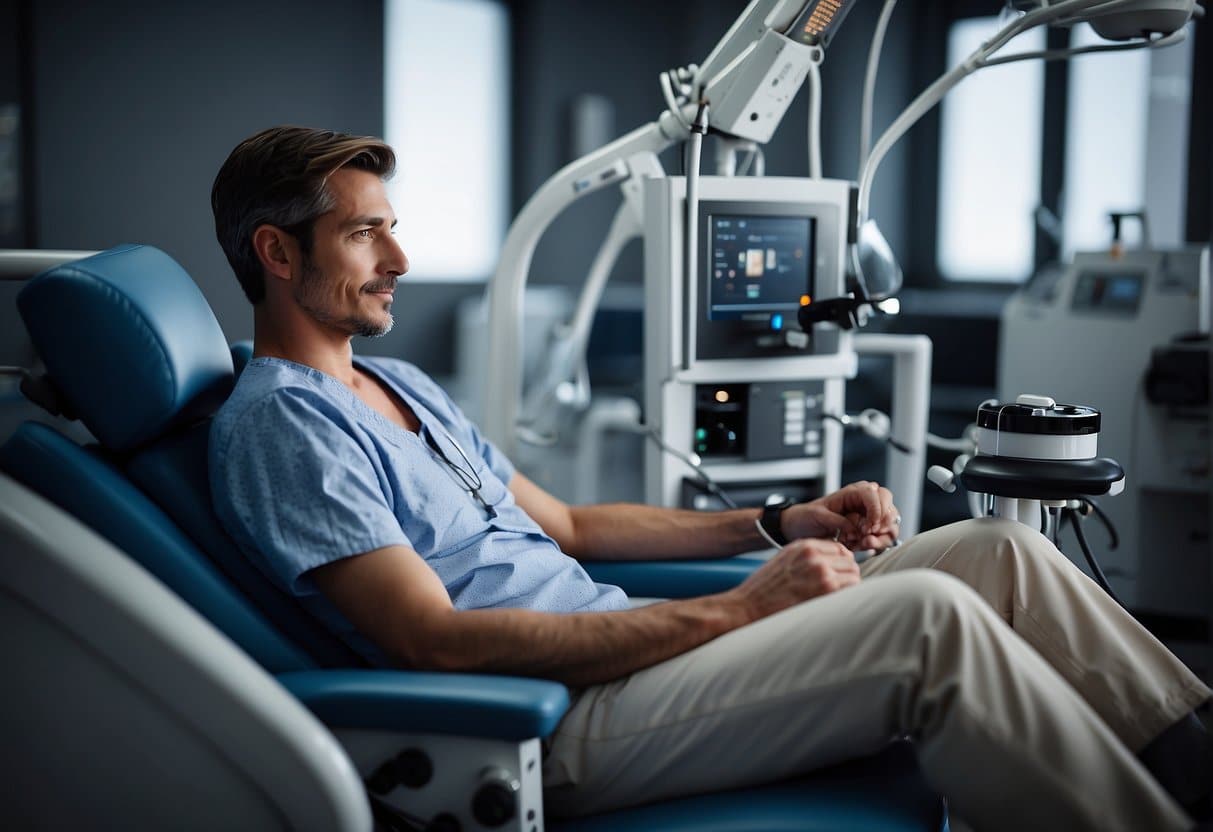
Kidney dialysis is a medical procedure designed to compensate for the loss of kidney function.
When kidneys are no longer able to perform their essential task of filtering waste products and excess fluid from the blood, dialysis takes on this role artificially. It’s a critical treatment for individuals with kidney failure, a severe condition often resulting from chronic kidney disease or acute kidney injuries.
Chronic kidney disease gradually diminishes kidney function over time, while acute kidney injury can cause sudden loss of function.
Both conditions may eventually progress to a point where kidney dialysis becomes necessary. In such cases, dialysis helps maintain a balance of body fluids and electrolytes, which are crucial for normal body operation.
Various treatment options are available, including hemodialysis, which is typically administered in a clinic or hospital, and peritoneal dialysis, which patients can often perform at home.
Quality of life for those on dialysis can vary, but treatment advancements continue to aim for improved outcomes.
Dialysis is integral for sustaining life in the absence of adequate kidney function, but it’s not a cure for kidney disease. As such, medical professionals are committed to managing side effects and coordinating with patients to ensure that treatment aligns with their lifestyle and health goals.
Emphasis is also placed on the potential for a kidney transplant, which for many is the preferred long-term solution for kidney failure.
Understanding Dialysis
Dialysis is a renal replacement therapy that performs the function of the kidneys by removing waste products and excess fluids from the blood when the kidneys are no longer able to do so effectively.
Types of Dialysis

There are two main types of dialysis: hemodialysis and peritoneal dialysis. Hemodialysis involves an artificial kidney, known as a dialyzer, to filter blood. This can be performed at home or in a clinic, known as home hemodialysis and in-center hemodialysis, respectively. Peritoneal dialysis utilizes the body’s own peritoneum as a filter. There are two forms: continuous ambulatory peritoneal dialysis (CAPD) and automated peritoneal dialysis (APD).
Dialysis Procedure
- Hemodialysis: Blood is routed through a machine where it passes across a filter, the dialyzer, before being circulated back into the body. A vascular access, such as a fistula or graft, provides entry into the patient’s bloodstream.
- Peritoneal Dialysis (PD): A catheter is planted in the abdomen to allow dialysate, a cleansing fluid, to flow into and out of the peritoneal cavity. The peritoneum acts as a filter whereby waste products and excess fluid are exchanged with the dialysate and then drained.
Risks and Complications
Hemodialysis: Patients may experience low blood pressure, muscle cramps, high blood pressure, fatigue, itchy skin, nausea, and sleep problems.
Peritoneal Dialysis: Complications include infection, blockage, hernia, weight gain, fluid overload, hypotension, and nausea. Continuous monitoring by a nephrologist is essential to manage these risks effectively.
Patients may need dialysis as a short-term intervention or as a bridge to a kidney transplant, which is a more permanent solution. Dialysis extends the lives of patients with kidney failure and helps maintain their quality of life by performing the essential functions of the kidneys.
Dietary and Lifestyle Considerations

Patients undergoing kidney dialysis need to make careful dietary choices and lifestyle changes to support their treatment and overall well-being.
Nutritional Management
Diet: A tailored meal plan is crucial for those receiving dialysis. It typically limits potassium, phosphorus, and sodium intake to help manage their levels in the blood. Patients should consult with a dietitian to design a diet that complements their dialysis treatment.
- Potassium: High levels may affect heart rhythm. Limiting foods like bananas, oranges, and potatoes is essential.
- Phosphorus: Excess may cause bone issues. Patients should avoid dairy products and nuts.
- Sodium: Overconsumption can lead to fluid retention and high blood pressure. Processed and canned foods are often high in sodium and should be consumed sparingly.
Fluids: Managing fluid intake is critical since the kidneys can no longer effectively remove extra fluids. This involves monitoring and restricting beverages and foods high in liquid content to prevent complications such as swelling and high blood pressure.
- Dialysis Fluid: The composition of dialysis fluid is carefully calibrated to remove wastes and extra fluids while maintaining healthy electrolyte levels.
Supplements and Medications: Patients may require vitamin and mineral supplements, but these should only be taken under a healthcare provider’s advice due to potential accumulation in the bloodstream. Certain medications may also need to be adjusted in dosage or timing.
Lifestyle Adaptations
Exercise: Engaging in routine physical activity can improve a patient’s quality of life, but it should be tailored to the individual’s ability and energy levels. Exercise helps with muscle strength, cardiovascular health, and overall well-being, so patients are encouraged to find activities that they enjoy and can maintain consistently.
Routine: Developing a routine around dialysis sessions can lend a sense of control and normalcy. Adhering to a consistent treatment schedule is important for the effectiveness of dialysis.
Support System: Building a strong support system through family, friends, and support groups can provide emotional comfort and practical help. Patients who have a network to share their experiences and challenges with often cope better with the lifestyle adaptations that dialysis necessitates.
Financial and Support Resources

Kidney dialysis can weigh heavily on a patient’s finances and emotional well-being. Resources are available to help ease this burden, ranging from insurance coverage to psychosocial support networks.
Coverage and Assistance
Patients undergoing kidney dialysis typically require substantial financial support. Medicare usually covers dialysis for eligible patients, including a portion of the costs for in-center and home dialysis treatments. Coverage includes the services provided by the dialysis care team which often comprises nurses, dietitians, and technicians. Additionally, Medicaid may offer assistance for eligible individuals, supplementing costs not covered by Medicare.
Costs associated with kidney dialysis are also often supported by private health insurance plans. It is crucial for patients to discuss with their care team and hospital financial advisors to understand the extent of coverage and out-of-pocket expenses. Considering the financial implications of dialysis, hospitals frequently have financial counselors who assist patients in navigating coverage and exploring assistance options.
Psychosocial Support
The emotional impacts of kidney dialysis, such as depression and anxiety, are recognized by healthcare providers. Psychosocial support is considered an essential component of comprehensive dialysis care. Resources include counseling services and support groups, which can be vital for patients to maintain their emotional well-being.
A dialysis care team often includes a social worker who can provide direct psychosocial support or refer patients to appropriate resources. Hospitals typically connect patients with peer support groups, where sharing experiences can alleviate feelings of isolation. Surgeons and other healthcare professionals also play a role in identifying signs of emotional distress and facilitating timely interventions.